Clinical Pearls in Optometry: Myopia Part 2
This second part of the Myopia series will cover clinical management guidelines and protocols, as well as various myopia management strategies and their efficacy

In the last part of this series we discussed the classification and risk factors of myopia. This second part will cover clinical management guidelines and protocols, as well as various myopia management strategies and their efficacy.
As mentioned in Part 1, it has been predicted that half the global population will be myopic by 2050, therefore intervention is imminent. Over the last 15 years, extensive research has been and continues to be carried out globally to find a plausible solution for the 'myopia epidemic'.

Based on the myriad of evidence of the prevalence and progression of myopia, the World Council of Optometry published a resolution for the "Standard of Care for Myopia Management by Optometrists" (above link). This implies that some form of myopia management is now considered the duty of care by the optometrist to their patient, where it would be considered negligent if myopia management is not provided when appropriate.
What is Myopia Management?
Myopia management is a proactive decision by the practitioner to take action to slow down the progression of myopia using evidence-based and clinically proven interventions. This does not include simple correction of myopia with spectacle lenses or contact lenses to improve the visual acuity. There is strong evidence to suggest that merely correcting the myopia WILL NOT slow down the progression. Furthermore, there appears to be a misconception among parents that their child should be slightly under-corrected to avoid myopia progression, however, there is no evidence to back this up, on the contrary, there is strong evidence that suggests that under-correction actually increases the rate of progression and is therefore contraindicated in myopic children. According to the International Myopia Institute publications, a clinically significant reduction in progression is 50%.
Interventions
The goal of myopia management is to reduce the progression of myopia and there is decades worth of conclusive evidence demonstrating that axial elongation is the key factor in the progression of myopia, hence reducing axial elongation is the best strategy for reducing the progression of myopia. All of the interventions are designed around this strategy and there is now strong evidence to suggest that multiple interventions implemented simultaneously can be more effective in cases where the myopia progression is aggressive, for example, in children where the onset of myopia is at an early age. The interventions fall into three categories: optical, pharmaceutical and environmental / behavioural. We will be discussing the principle, efficacy, safety and implementation of all of the aforementioned interventions.
Pharmaceutical Interventions
Principle: Pharmaceutical interventions for slowing down the progression of myopia have been in place for some years. The pharmaceutical agent most commonly used is Atropine. Atropine is a broad-spectrum anti-muscarinic agent, which blocks muscarinic acetylcholine receptors in smooth ocular muscle with parasympathetic innervation. This results in cycloplegia (total relaxation of accommodation) and mydriasis (pupil dilation). The initial reasoning behind using atropine for myopia control was due to the belief that relaxing accommodation reduces axial elongation and the positive efficacy of the drug was a result of cycloplegia. However, recent animal studies have shown that this is not the case and in actuality, it is a possible effect of the atropine mainly on retina and the sclera that reduces axial elongation, with some contributing factors from the retinal pigment epithelium and the choroid. Atropine may increase the dopamine production in the retina and dopamine agonists inhibit myopia progression. At the level of the sclera, animal studies have suggested that atropine increases the thickness of the scleral fibrous layer in myopic eyes, reducing axial elongation.
Efficacy: Most literature agrees that atropine is the most effective intervention in reducing myopia progression, ranging from a 70% to 12% reduction in progression depending on the dose, with higher doses demonstrating a greater reduction. The LAMP study, published recently, investigated to efficacy of low dose atropine: 0.05%, 0.025% and 0.01%. The outcome was a clinically significant reduction in myopic progression, with virtually no side effects after 24 months.
Safety: Conventional doses of atropine used for diagnostic purposes have short side effects such as blurred vision, glare and photophobia and long term exposure to excessive amounts of UV radiation, all of which can significantly affect a child's quality of life. However, the LAMP study demonstrated that low dose atropine is effective without any impace on quality of life. The only draw back to low dose atropine as an method of myopia management is a significant rebound effect as compared to optical interventions, which has been demonstrated in several studies.
Implementation: Low dose atropine (0.01%) is approved as a method of myopia management by the Indian FDA, however, it is still prescribed off-label in most other countries. It is also a prescription-only medication, which can prescribed by a medical practitioner only. Therefore, Optometrists that wish to put their patients on low dose atropine would have to do it in co-management with an ophthalmologist.
Optical Interventions
Principle: Early researchers in the contact lens field believed that myopic progression occurred due to corneal steepening during development and there were a few publications that loosely claimed rigid lenses could slow down the progression of myopia, although this was probably found in cases where the cornea was flattened due to the rigid lens. Modern rigid lens designs tend not to cause corneal flattening or spectacle blue. This theory was disregarded when it was found that myopic progression is actually due to axial elongation that occurs during development, instead of emmetropization. Recent literature revealed that the main cause of axial elongation is peripheral hyperopia, where when the myope is corrected with spectacles or regular contact lenses, while the central image is may be on the retina, the peripheral rays of light focus behind the retina, causing peripheral hyperopia, as demonstrated in Figure 1.
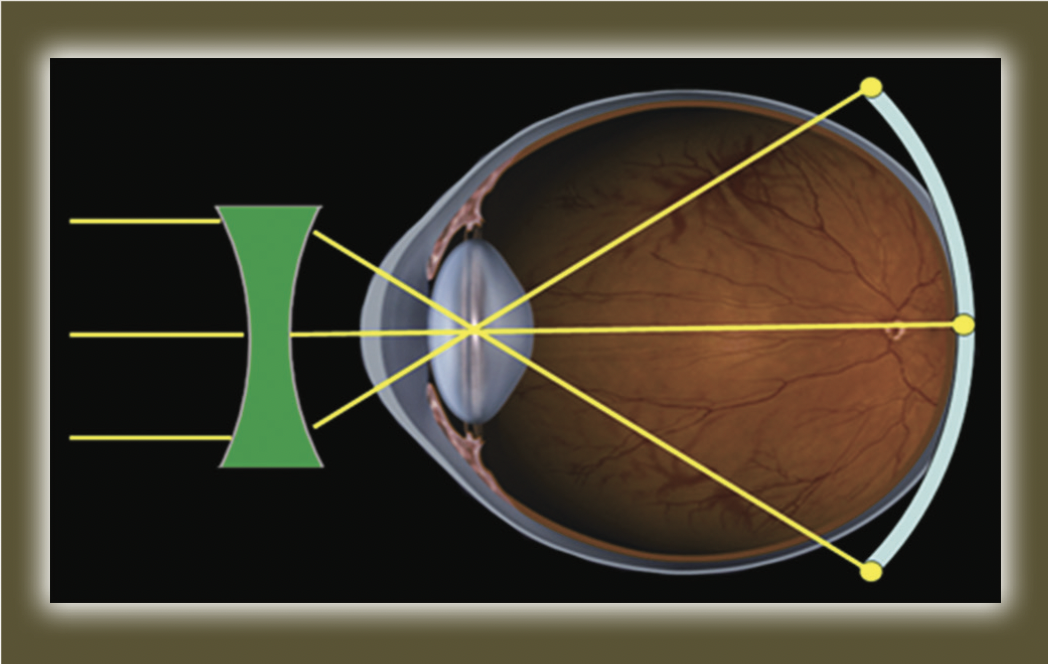
Peripheral form deprivation due to peripheral hyperopia, stimulates elongation of the axial length. This was demonstrated in primates, where once the peripheral hyperopia was eliminated, the eye became emmetropic, even in cases where the fovea was ablated. This indicates the magnitude of the role of peripheral hyperopia in myopic progression and based on this evidence, one could conclude that eliminating peripheral hyperopia may slow down the progression of myopia.
Efficacy: Optical interventions include Orthokeratology or Corneal Reshaping contact lenses, centre distance multifocal and extended depth of focus (EDOF) soft contact lenses and, more recently, specially designed spectacle lenses for myopia management. There is enough literature to provide strong evidence demonstrating that Orthokeratology and multifocal / EDOF soft contact lenses result in approximately 50% reduction of myopia progression. As far as spectacle lenses are concerned, the literature is limited, although initial reports are very promising, demonstrating approximately 65% control of axial elongation in the duration of the studies, however further publications will provide a better idea of control over a longer period of time. The two main designs that are being researched extensively are Highly Aspheric Lenslet Target (H.A.L.T) and Defocus Incorporated Multiple Segments (DIMS).
Safety: The safety of contact lens wear in young children is frequently questioned by practitioners. Modern rigid lens materials providing excellent oxygen permeability allow safe overnight wear of contact lenses, without virtually no incidence of hypoxia related complications. Studies have shown that the incidence of microbial keratitis was most common in East Asian countries, where Pseudamonas and Acanthamoeba were the primary micro-organisms causing the infections. It was concluded that the reasons behind these incidences included poor adherence to care regimes, as well as use to tap water to rinse the lenses. Similarly, when it comes to soft contact lenses, typically daily replacement lenses would be considered the safest as compared to a daily reusable lens, however for any contact lens wearer, child, teenager or adult, a combination of proper instruction from the eye care practitioner as well as strict adherence to the prescribed care regimen and regular follow up appointments minimise the risk of complications.
Implementation: Spectacles are the least invasive method for myopia management, however, correct myopia protocols must be followed for all optical interventions for myopia. Peripheral defocus soft contact lenses as well as orthokeratology require a level of training and expertise in contact lens fitting, but are excellent options for children who don't want to wear spectacles for any number of reasons including self esteem issues or sports and other leisure activities. All optical myopia management strategies do come at a higher cost compared to conventional spectacles and contact lenses, which is something that must be considered while counselling the patient.
Environmental / Behavioural Interventions
As discussed in the previous post, the amount of time spent out doors and working distances can considerably increase the risk of myopia progression. Therefore counselling the parents and the children on behavioural and environmental interventions is essential. These interventions include monitoring the working distance at which the child is carrying out near tasks and the amount of time spent at a stretch for near tasks. The International Myopia Institute clinical management guidelines suggest that the working distance should not be less than 20cm and time spent should not exceed 45 minutes at stretch. This does not mean that the child must not perform near tasks, but regular breaks are indicated, where the fixation is taken away from the near task. Similarly the guidelines suggest that a minimum of 8 hours should be spent outside during daylight hours to reduce the risk of myopia progression. The implementation of these guidelines should be the minimum responsibility of any eye care practitioner that has a myopic child under their care.
Myopia Management Protocol
- History Taking: Identify the risk factors of myopia development or progression
- Cycloplegic or Non-Cycloglegic: Ensure that correct measures are taken to ensure that the accommodation is relaxed during refraction
- Record Best Corrected Visual Acuity
- Binocular Vision Function: Accommodative lead/lag, Accommodative Facility with +/- 2.oo flipper, Amplitude of Accommodation, Distance and Near Heterophoria evaluation and AC/A Ratio should all be measured for baseline values before commencing and myopia therapy. If values for any of the above are outside of normal, this must be addressed before commencing myopia therapy. All of the above should be monitored on a regular basis after commencing myopia therapy
- Anterior and posterior segment evaluations: Especially important if prescribing contact lenses and should be monitored carefully in all myopes to screen for pathologic myopia
- Tear Film Evaluation: Particularly important if prescribing contact lenses.
- Axial length: The most accurate way to monitor progression, should be measured at baseline and every six months thereafter. The ideal instrumentation for axial length measurement is non-contact optical biometry.
- Corneal topography: In the absence of an optical biometry, the combination of corneal topography with an accurate refraction is another way to monitor progression. Corneal topography is also necessary for orthokeratology.
- Selection of appropriate intervention: Based on patient history, age of onset of myopia and assessed risk of progression
- Clear patient counselling: Advice on risks of progression and importance of intervention. Counselling on behavioural and environmental interventions to reduce progression.
Conclusion
Myopia management is on course to become a normal optometric practice, so it is important for all eye care professionals to familiarise themselves with all the interventions and correct protocols. The Asira Electronic Medical Record platform allows detailed documentation for the myopia management protocols.
ASIRA is a simple and secure, cloud-based software tool, built BY optometrists FOR optometrists, that helps eye care professionals reduce the time and effort required to maintain clinical records, schedule appointments, generate bills, manage inventory and much more!
To find out more, visit www.asira.health and sign up for a 30-Day FREE TRIAL! If you're a new practice owner or a fresh graduate thinking of entrepreneurship, visit www.asira.health/optompreneur to learn how ASIRA can help reduce your costs and increase revenue.



Comments ()