Clinical Pearls in Optometry: Myopia Part 1

In 2016, the Late Brien Holden and his colleagues published a paper that shook the eye care field across the world. The paper concluded that by 2050, 50% of the world's population will be myopic, making myopia the leading cause of preventable visual impairment in the world. In its World Report on Vision, the World Health Organisation recognises myopia to be one of the five conditions that are currently contributing to visual impairment across the globe. Since then, eye care practitioners globally have shifted into fifth gear to tackle what is being lovingly referred to as 'The Myopia Epidemic'. This series of articles will cover all the latest research in Myopia Management, including classification and risk factors of myopia, as well as the various myopia management strategies, their protocols and efficacy to help you choose the strategies most suitable for you to implement in your practice.
Definition and Classification of Myopia
The current World Health Organisation definition of myopia is as follows:
"A refractive error in which light rays entering the eye parallel to the optic axis are brought to focus in front of the retina when accommodation is relaxed. This results from an overly curved cornea or from the eyeball being too long from front to back. It is also called nearsightedness."
While the definition exists, and myopia has been acknowledged by WHO, to be a definite public health concern, there is no validated, universally recognised classification system for myopia, such as those that exist for Diabetic Retinopathy or Retinopathy of Prematurity. Daniel Flitcroft and colleagues published a paper in 2018, proposing a system where myopia can be defined qualitatively, quantitatively and descriptively.
Qualitative definitions: The qualitative definitions refer to the physiological reason behind the development of myopia. This is essential in determining the best strategies for monitoring the progression and managing myopia.
Axial Myopia: "a myopic refractive state that can be attributed to excessive axial elongation": Myopia as a result of a longer than average eye ball
Refractive Myopia: "a myopic refractive state that can be attributed to changes in the structure or location of the image forming structures of the eye": Myopia as a result of higher than average corneal curvature and/or higher than average power of the crystalline lens
Secondary Myopia: "a myopic refractive state for which a single, specific cause can be identified that is not a recognised population risk factor for myopia development": Myopia as a result of a specific underlying cause, which does not fall under the normal risk factors for the development of myopia; this may include an adverse drug event, a corneal abnormality or a systemic condition
Quantitative Definitions: The quantitative definitions refer to the degree of myopia present. This is necessary to assess the risk of further complications that may lead to visual impairment. All of the below quantitative definitions refer to the spherical equivalent refractive error (sphere + 1/2 cylinder) of an eye, when ocular accommodation is relaxed.
Myopia: Equal to or more than -0.50D
Low Myopia: -0.50D to (but not including) -6.00D
High Myopia: Equal to or more than -6.00D
While we are all familiar with the terms 'Low Myopia' and 'High Myopia', the paper proposed an additional quantitative definition:
Pre-Myopia: +0.75D to (but not including) -0.50D "in children where a combination of baseline refraction, age, and other quantifiable risk factors provide a sufficient likelihood of the future development of myopia to merit preventative interventions": According to the CLEERE Study, quantifiable risk factors may include accelerated axial elongation and low or no hyperopia in children compared to age-matched normative data. Furthermore, other well- documented risk factors such as a positive family history of myopia and environmental factors such as time spent indoors or outdoors may also warrant intervention.
Descriptive Definitions: The descriptive definitions refer to the complications caused as a result of a high degree of myopia with the absence of any other underlying condition.
Pathologic Myopia: This is an encompassing term, referring to pathology, which is a result of excessive axial elongation, resulting in deterioration of visual acuity, which may eventually lead to visual impairment. Pathologic Myopia includes:
- Myopic Macular Degeneration (MMD)
- Myopic Traction Maculopathy (MTM)
- Myopia-Associated Glaucoma-like Optic Neuropathy
Risk Factors of Myopia Development and Progression
It is important to understand the risk factors of the development and progression of myopia in order to plan interventions, whether that involves advice on lifestyle and habits or exploring methods of myopia control. It is well documented that there are both genetic and environmental factors that contribute to the development and progression of myopia and while there have been several suggested risk factors, there is strong evidence suggesting four risk factors that have a strong contribution to causality.
- Parental myopia: The literature suggests that the probability of the inheritance of myopia is around 60-80%, suggesting that there is definitely a genetic element. In addition to this, there is a strong possibility that the child's lifestyle and environment will also mimic that of the parents, which is most probably a myopiagenic environment, resulting in an additional contribution, beyond just genetics, to the overall development or progression of myopia in the child.
- Education: There is an abundance of literature supporting the fact that there is a very strong correlation between education and the prevalence and progression of myopia in children:
- Myopia is more prevalent among communities where the children attend school versus those where they don't
- Children who are more academically orientated tend to be myopic and a high performance in school precedes myopia
- Myopia is more prevalent among adults who spent more years in academic institutions
- Countries that have a high prevalence of myopia also have schooling systems with more academic pressure, for example, homework and examinations start at a much younger age
As mentioned above, it is well documented that educational pressure does contribute to the development and progression of myopia, however, the reasons behind this are much debated. Some studies have found a clear relationship between near work and the progression of myopia and arguably, children in school spend more time reading and writing, which could be a contributing factor. Initially it was suggested that the accommodative lag that was a result of continuous near work triggering myopic progression, but more recent animal studies have shown that hyperopic defocus stimulates axial elongation and myopic progression.
3. Time Spent Outdoors: Strong evidence has been produced supporting the fact that 40-80minutes of time spent outdoors significantly reduces the incidence of myopia. This has been attributed to the increased production of dopamine due to exposure to bright light during time spent outdoors in the daytime, which appears to inhibit axial elongation. Other studies have also shown that myopic children and teenagers exhibited reduced Vitamin D levels, which would be a result of lack of exposure to sunlight, therefore increasing the time spent outdoors, increased vitamin D levels and in turn should slow down the progression of myopia. The exact mechanism of the relationship between time outdoors and myopia is yet to be fully understood, but it is clear and conclusive that this relationship exists. Therefore, advising parents about adopting this lifestyle change is an integral part of myopia management.
4. Axial Length (AL) and Spherical Equivalent Refraction (SER): The Northern Ireland Childhood Errors of Refraction (NICER) Study and The Singapore Cohort of the Risk Factors for Myopia (SCORM) are two studies carried out at opposite ends of the globe. NICER included a Western European White population, while SCORM included primarily East and South Asian populations. The data from both NICER and SCORM was in agreement that the earlier the onset of a long AL and a myopic SER, the higher the rate of progression of myopia.
The data from NICER and SCORM, as well as several other longitudinal studies, has enabled eye care practitioners to make logical predictions when it comes to the incidence and rate of progression of myopia. With the data from the NICER Study, colleagues at Ulster University were able to create the Predicting Myopia Onset and Progression (PreMo) risk factor indicator:
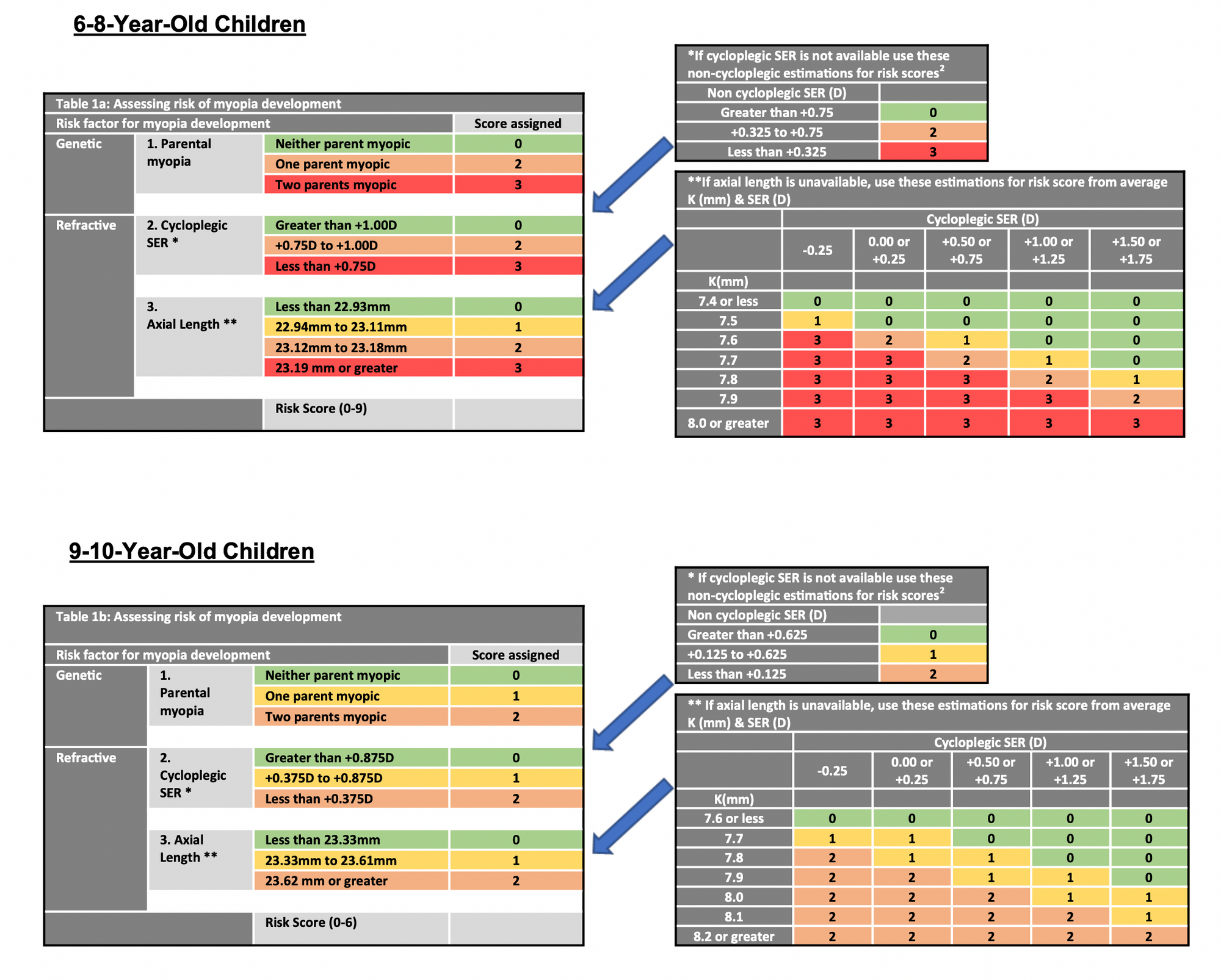
While PreMo is based on a white Western European population, the prevalence of myopia in the United Kingdom is not completely dissimilar to that of South Asian Urban populations, so it can certainly be used as a guideline for risk assessment and management strategies.
Conclusion
Armed with evidence based knowledge of the classification and risk factors of Myopia, eye care practitioners can confidently and competently manage myopia in children. The next part in this series will explore various guidelines and protocols for myopia management, as well as look into different interventional strategies for myopia control.
ASIRA is a simple and secure, cloud-based software tool, built BY optometrists FOR optometrists, that helps eye care professionals reduce the time and effort required to maintain clinical records, schedule appointments, generate bills, manage inventory and much more!
To find out more, visit www.asira.health and sign up for a 30-Day FREE TRIAL! If you're a new practice owner or a fresh graduate thinking of entrepreneurship, visit www.asira.health/optompreneur to learn how ASIRA can help reduce your costs and increase revenue.


Comments ()