Clinical Pearls in Optometry: Dry Eye Disease - Part 1.
Dry Eye Disease (DED) is a common ocular surface condition, due to disruption of the tear film. This series will cover classification, etiology, pathophysiology and management strategies of DED.

Dry Eye Disease (DED) is common ocular surface condition affecting approximately 30% of the global population, according to a recent review by Eric Papas. DED is a result of disruption of the natural tear film, the cause of which is multifactorial. This series of articles will cover classification, etiology, pathophysiology and effective management strategies DED.
Anatomy and Physiology of the Tear Film
The tear film is location anterior to the cornea and conjunctiva, as shown in Figure 1, and plays an essential role in maintaining the integrity of the ocular surface. The composition of the tear film is complex, with each component having its respective function.
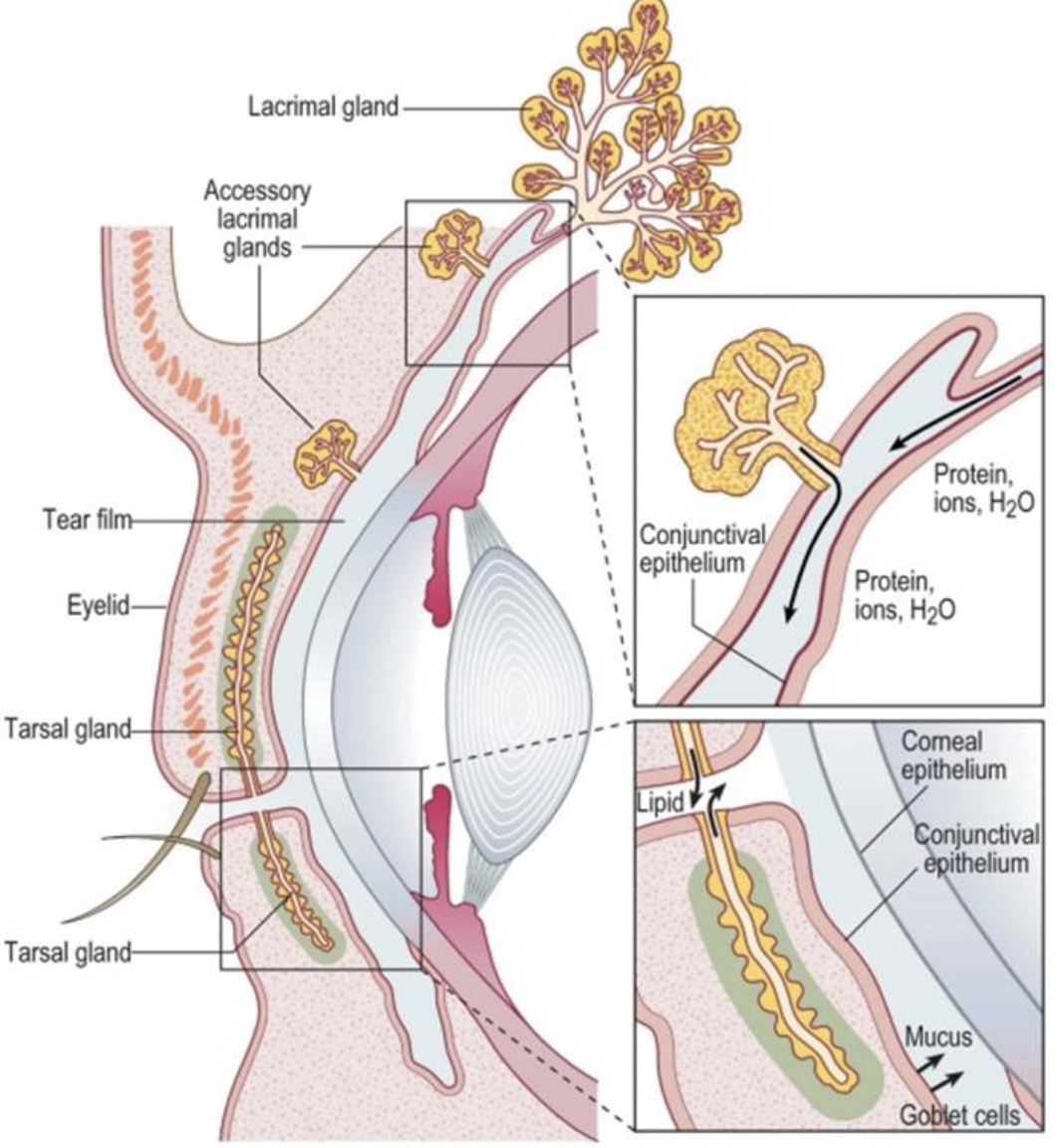
The tear film has four important functions:
Optical: With every blink, the tear film spreads evenly over the surface of the eye ensuring a smooth optical surface. DED can cause disruption in this function, resulting in intermittent blurred vision.
Metabolic: The tear film refreshes with every blink, which is referred to as 'tear turnover'. For the cornea to maintain transparency, it is a completely avascular surface and therefore relies on atmospheric oxygen for metabolism. The tear turnover enables the tear film transmits the oxygen from the atmosphere to the cornea via gaseous exchange, as well as removing metabolic waste.
Protection: "Reflex tearing" is term used to describe hyper-secretion of the tear film when a foreign substance is detected on the ocular surface, enabling the mechanical removal or flushing of the foreign substance and prevents microbial adhesion to the ocular surface. In addition to this, the film contains several antimicrobial proteins, such as IgA, lysozyme, lactoferrin and lipocalin, which all have bacteriocidal properties.
Lubrication: The non-Newtonian property of the tear-film ensures that the surface friction across the ocular surface remains low at all times, to protect the corneal epithelium.
The tear film has three main components, structured in a laminar fashion. The most anterior layer is called the lipid layer. It consists of a clear oil, which is secreted from the meibomian glands, located inside the upper and lower eyelids, within the tarsal area of the eyelid. The meibum is secreted onto the eyelid margin and spreads across the ocular surface with every blink. The main function of the lip layer is to create a hydrophobic barrier, which prevents the aqueous component of the tear film from evaporating. The aqueous component, which lies directly under the lipid layer and consists mostly of water, metabolites and antimicrobial proteins. It contributes largely to the overall functions of the tear film, therefore must be preserved. The aqueous is secreted by the lacrimal gland. Finally, the most posterior layer is the mucin layer, secreted from the goblet cells in the conjunctiva. Mucin consists of high molecular weight glycoproteins, which play an essential role in anchoring the tear film to the cornea and conjunctiva behind it as well as ensuring the tear film spreads evenly across the ocular surface.
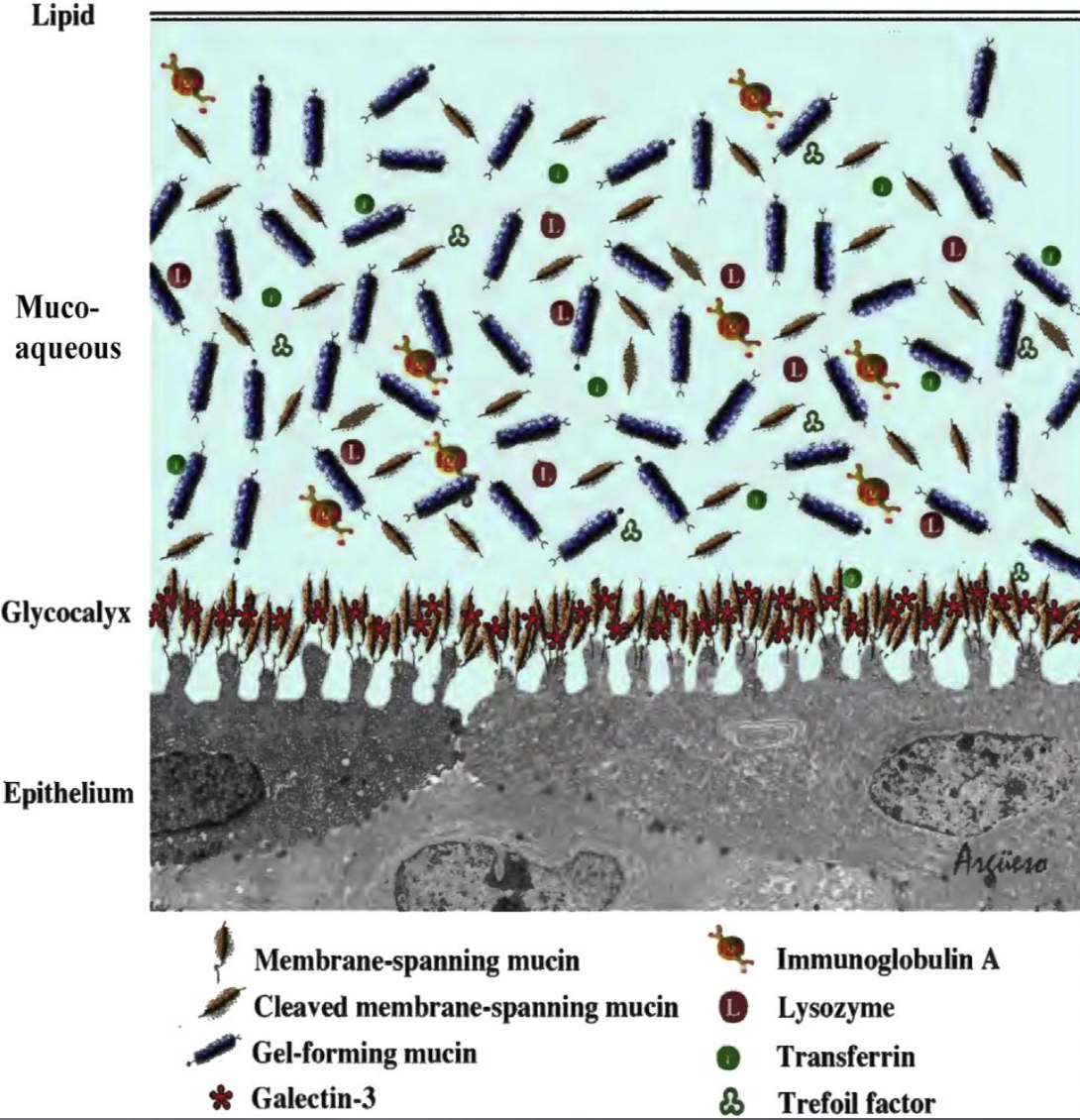
Definition and Classification of Dry Eye Disease
The definition of DED has evolved over the years as studies continue to reveal new aspects of this complex multifactorial condition. The current definition, published by TFOS DEWS II states:
"Dry eye is a multifactorial disease of the ocular surface characterised by a loss of homeostatis of the tear film, and accompanied by ocular symptoms, in which tear film instability and hyperosmolarity, ocular surface inflammation and damage, and neurosensory abnormalities play etiological roles."
Since the above definition clearly indicates the complex nature of the condition, it is imperative that the disease is correctly identified, classified and diagnosed in order to ensure an excellent treatment plan. The first TFOS DEWS report, published in 2007, had two main classifications of dry eye, based on basic pathophysiology, which influences the behaviour of the tear film, followed by a few sub-classifications. The main classifications were Aqueous Deficient Dry Eye (ADDE) and Evaporative Dry Eye (EDE). ADDE refers to a type of dry eye, which is a result of reduced production of aqueous from the lacrimal gland. Further sub-classifications in this category included Sjogren Sydrome Dry Eye (Primary and Secondary) and Non-Sjogren Dry Eye (Lacrimal Deficiency, Lacrimal Gland Duct Obstruction, Reflex Block, Systemic Drugs). EDE refers to a type of dry eye where aqueous production is normal, however the tears are evaporating from the ocular surface. Further subclassifications in this category included Intrinsic (Meibomain Oil Deficiency, Disorders of the Lid Aperture, Low Blink Rate, Drug Action Accutane) and Extrinsic (Vitamin A Deficiency, Topical Drug Preservatives, Contact Lens Wear, Other Ocular Surface Disease e.g. Allergy). EDE is typically more common than ADDE.
While this classification is not at all inaccurate, it may be considered inadequate, as more recent research has shown that there may be a considerable amount of overlap between the two categories, especially when one considers the external environment to which the eyes are being exposed. TFOS DEWS II research has resulting in the introduction of a much more comprehensive protocol for the classification of dry eye, which is based on presenting symptoms, signs and triaging question, which will lead to THREE categories (contrary to the previous report, which stated TWO categories): 1. Aqueous Deficient Dry Eye 2. Mixed Dry Eye 3. Evaporative Dry Eye. This new classification protocol, will enable practitioners to navigate the management of dry eye much better than before. The detailed TFOS DEWS II Definition and Classification Report published by Dr. Jennifer Craig and colleagues is available in The Ocular Surface 15 (2017) 276-283.
Pathophysiology of Dry Eye Disease
The TFOS DEWS II Pathophysiology Report published by Anthony Bron and colleagues revealed that there are several physiological changes that occur in the tear film that contribute to dry eye disease, including tear film hyperosmolarity, corneal epithelial barrier disruption, ocular surface friction and epithelial cell desquamation. All of these factors combined can contribute to asymptomatic or symptomatic dry eye disease, and they all may exist in Aqueous Dry Eye, Mixed Dry eye AND Evaporative Dry Eye.
Tear film hyperosmolarity is one of the main cascading events that leads to symptomatic dry eye disease. A normal tear film has an average osmolarity of 3o2 mOsm/L, the average value for mild to moderate DED 316 mOsm/L and for severe DED is 336 mOsm/L. Factors causing tear film hyperosmolarity include body dehydration, a compromised tear film lipid layer (causing fast evaporation of tears), low blink rate, larger palpebral aperture size, tear film instability and ambient environmental conditions such as low humidity and windiness.
When the corneal epithelium is exposed to hyperosmolarity, it triggers a cascade of inflammatory mediators and enzymes, in particular matrix metalloproteinases (MMPs), which promote the disruption of intercellular tight junctions in the corneal epithelium as well as epilthelial cell apoptosis, disrupting the corneal epithelial barrier. The presence of MMP9 in the tear film, is a key marker of DED.
Increase in ocular surface friction can become symptomatic as the lids pass over the ocular surface. This is a result of reduced lubrication due to damage to the glycocalyx, which anchors the mucin layer to the corneal epithelium. Increased ocular surface friction may also result in lid wiper epitheliopathy and superior limbic keratoconjunctivitis.
Finally, all of the above contribute to epithelial cells desquamation both in the cornea and the conjuntiva. This refers to the separation of the layers of the squamous cells in the corneal epithelium, which will present as corneal staining.
Bron and Colleagues went on to demonstrate what they described as "The Vicious Circle of Dry Eye Disease", where each of these physiological changes leads to the next one starting with hyperosmolarity, which causes disruption of the corneal epithelial barrier, which in turn increases ocular surface friction, resulting in epithelial desquamation and tear film instability, which of course increases osmolarity, hence completing the circle. This revelation was one of the main reasons behind TFOS DEWS II suggesting a new classification protocol. These protocols provide practitioners with a systematic approach to investigating and managing DED appropriately. The next and final article in this series will cover investigation and management of DED.
ASIRA is a simple and secure, cloud-based software tool, built BY optometrists FOR optometrists, that helps eye care professionals reduce the time and effort required to maintain clinical records, schedule appointments, generate bills, manage inventory and much more!
To find out more, visit www.asira.health and sign up for a 30-Day FREE TRIAL! If you're a new practice owner or a fresh graduate thinking of entrepreneurship, visit www.asira.health/optompreneur to learn how ASIRA can help reduce your costs and increase revenue.


Comments ()